

Assessing Antibody Levels in Long COVID Patients: Insights from Okayama University Study
Assessing Antibody Levels in Long COVID Patients: Insights from Okayama University Study
In the wake of the COVID-19 pandemic, the need for effective treatment of long COVID symptoms, especially among those affected by the Omicron variant, has prompted extensive research. A recent study conducted by a team from Okayama University has revealed significant correlations between SARS-CoV-2 antibody levels and the severity of long COVID symptoms, specifically brain fog and diminished quality of life (QOL).
Overview of the Study
Carried out between July 2023 and November 2024, the research involved analyzing 275 patients who visited Okayama University's COVID Aftercare Clinic. The participants, consisting of 146 females and 129 males with a median age of 41, were evaluated for their levels of anti-spike (S) and anti-nucleocapsid (N) antibodies in their serum. The study aimed to explore how these antibody levels correlated with clinical symptoms and individual backgrounds.
Key Findings
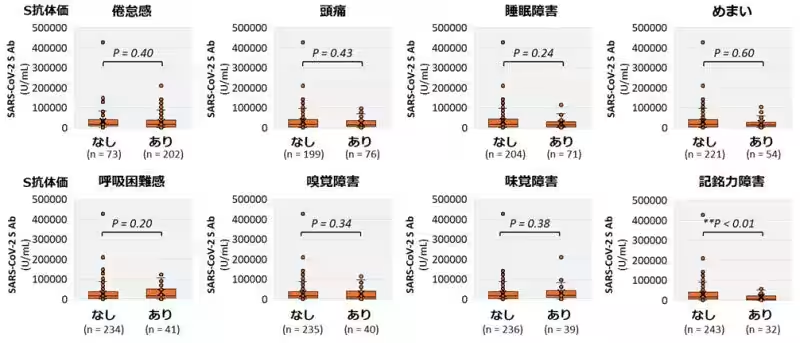
The findings indicate that patients with lower levels of S antibodies displayed notable cognitive issues, often characterized as brain fog, alongside lower overall quality of life. Conversely, those with higher N antibody levels, particularly women and individuals who experienced severe illness during their COVID-19 infection, demonstrated elevated antibody concentrations. Notably, the study found that N antibodies tend to diminish over time post-infection, supporting the notion that these measurements could serve as valuable biomarkers for understanding long COVID outcomes.
Implications for Long COVID Treatment
The inability to objectively measure the status of long COVID has been a long-standing challenge, primarily because symptoms like fatigue, headaches, and sleep disturbances can be subjective and varied among individuals. However, this study highlights the potential of using antibody levels to better evaluate the prognosis of long COVID patients, particularly in the context of different variants of the virus. By understanding the relationship between antibody levels and patient symptoms, healthcare professionals may be able to develop more tailored treatment plans.
In their statement, Marina Kawaguchi, the lead researcher, expressed the importance of establishing a link between immune responses post-infection and the persistence of cognitive deficits associated with long COVID, wishing that the findings would enhance the understanding of brain fog’s pathology in these patients.
Additionally, Taiyo Sakurada from the research team emphasized the progress made towards clarifying long COVID’s underlying mechanisms and the establishment of reliable biomarkers. He reiterated the commitment to creating evidence that can directly aid in patient recovery.
Professor Kazuki Tokumasu added to this by noting that, while cases of COVID-19 have decreased, the number of patients requiring long-term care for lingering symptoms remains high. The importance of ongoing research and clinical attention to long COVID is crucial given its continuing impact on a significant portion of the population.
Publication and Future Research
The results of this comprehensive study have been published in the British Journal of Biomedical Science on April 22, 2026. The article, titled "Clinical Utility of SARS-CoV-2 Antibody Titers in the Management of Patients with Long COVID Infected with the Omicron Variant," highlights the need for advanced research to further validate these findings and explore the clinical applications of antibody measurements in long COVID treatment.
As researchers continue to unravel the complexities of COVID-19, studies like this one at Okayama University underline the necessity for innovative approaches to patient care in the aftermath of the pandemic. These insights are not only significant for Japan but could also contribute globally to the understanding and treatment of long COVID.









Topics Health)









【About Using Articles】
You can freely use the title and article content by linking to the page where the article is posted.
※ Images cannot be used.
【About Links】
Links are free to use.